|
Inhibition of endothelial cell activation by b. HLH protein E2- 2 and its impairment of angiogenesis. Abstract. E2- 2 belongs to the basic helix- loop- helix (b. HLH) family of transcription factors. E2- 2 associates with inhibitor of DNA binding (Id) 1, which is involved in angiogenesis. In this paper, we demonstrate that E2- 2 interacts with Id. Mutational analysis revealed that the HLH domain of E2- 2 is required for the interaction with Id. In addition, Id. 1 interfered with E2- 2–mediated effects on luciferase reporter activities. Interestingly, injection of E2- 2–expressing adenoviruses into Matrigel plugs implanted under the skin blocked in vivo angiogenesis. In contrast, the injection of Id. E2- 2–mediated inhibition of in vivo angiogenic reaction. Consistent with the results of the Matrigel plug assay, E2- 2 could inhibit endothelial cell (EC) migration, network formation, and proliferation. On the other hand, knockdown of E2- 2 in ECs increased EC migration. The blockade of EC migration by E2- 2 was relieved by exogenous expression of Id. We also demonstrated that E2- 2 can perturb VEGFR2 expression via inhibition of VEGFR2 promoter activity. This study suggests that E2- 2 can maintain EC quiescence and that Id. Introduction. Angiogenesis is the formation of new vessels from preexisting ones by sprouting or by intussusceptive microvascular growth. Angiogenesis takes place throughout development as well as in adulthood. Although the vasculature in adults is generally quiescent, angiogenesis occurs to ensure physiologic homeostasis and integrity after wound healing, inflammation, ischemia, and during the female reproductive cycle. Angiogenesis encompasses 2 phases: activation and resolution. The activation phase is initiated by growth factor signals (eg, vascular endothelial growth factor . In this process, endothelial cells (ECs) proliferate, vascular permeability increases, and extracellular matrix components are degraded. These serial events allow ECs to migrate and form new capillary sprouts. During the resolution stage, ECs cease proliferation and migration, the basement membrane is reconstituted, and the vessels mature. The transition from the activation phase to the resolution phase, and vice versa, is referred to as the “angiogenic switch” and is determined by a tightly regulated balance between angiogenic inducers and inhibitors. 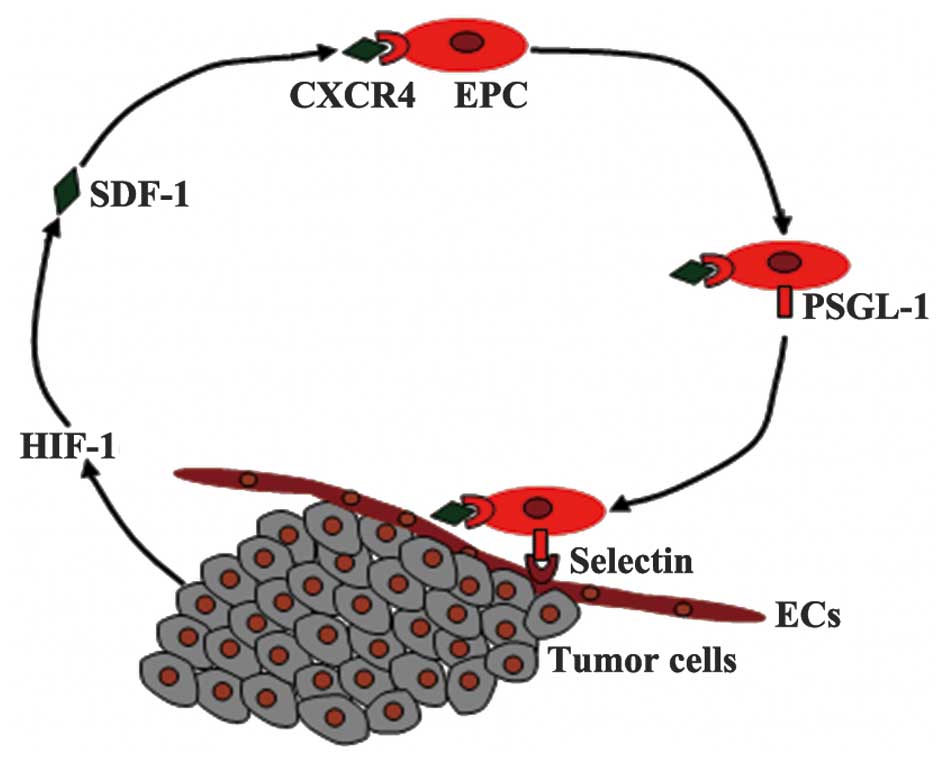  
Tetramethylpyrazine inhibits tumor growth of lung cancer through disrupting angiogenesis via BMP/Smad/Id-1 signaling. Authors: Youchao Jia; Zhigang Wang. Ablation of the transcriptional regulator Id1 enhances energy expenditure, increases insulin sensitivity, and protects against age and diet induced insulin resistance. This article reviews the evidence for macrophages playing an important role in the regulation of tumor angiogenesis. Findings in mouse models show that macropha. An angiogenesis inhibitor is a substance that inhibits the growth of new blood vessels ( angiogenesis). Some angiogenesis inhibitors are endogenous and a normal part.
The inhibitor of the DNA- binding (Id) family of proteins, consisting of Id. Id. 2, Id. 3, and Id. HLH) family of transcription factors. The basic HLH (b. HLH) family of transcription factors regulates transcription by binding to DNA as either homodimers or heterodimers. Id proteins, which lack a DNA- binding domain, interact with b. HLH proteins to prevent dimer formation and/or DNA binding. In addition, Id. 1 can associate with members of the Ets protein family and Rb. Several observations support a crucial role for Id proteins in development, differentiation, and proliferation of cells, and in tumorigenesis. For example, it has been demonstrated that Id. Myo. D- mediated myogenic responses. Id. 1/Id. 3 double- knockout mice display abnormal angiogenesis characterized by enlarged, dilated blood vessels. Introduction of Id. ECs induces EC proliferation and migration. Because knockdown of Id. ECs treated with BMP perturbs EC activation, Id. BMP- induced EC activation. Loss of Id. 1 in tumor ECs leads to down- regulation of integrin . Although many b. HLH transcription factors have been implicated in EC angiogenic activities, which proteins Id. We have reported that Hey. Herp. 2/Hesr. 1, one of the b. HLH proteins induced by Notch signaling, antagonizes activated BMP receptor- induced EC migration. This antagonism is caused by the degradation of Id. Hey. 1/Herp. 2/Hesr. ECs. Thus, Id. 1- induced EC migration is blocked by Hey. Herp. 2/Hesr. 1. 2. However, the mechanism by which Id. EC angiogenic activation is still poorly understood. To gain more insight into the molecular mechanisms by which Id. EC activation, we searched for Id. E2- 2. E2- 2 (also known as ITF2, TCF4, SEF2, and SEF2- 1. B) is classified into the E- protein family (or the class A type of b. HLH transcription factors), whose expression is virtually ubiquitous. In addition to E2- 2, E2. A and HEB also belong to the E- protein family. This family of transcription factors recognizes a consensus DNA sequence known as the E- box (CANNTG) in dimer form, whereas monomeric forms have no discernible DNA- binding activity. The E- protein family of proteins is known to regulate lymphocyte development,2. Our previous study demonstrated that E2- 2 can inhibit the activity of VEGFR2 luciferase reporters in ECs. However, how E2- 2 counteracts the activity of the VEGFR2 promoter and whether E2- 2 influences the actions of ECs remain veiled. In this study, we explored the role of E2- 2 in angiogenesis both in vitro and in vivo. We found that E2- 2 represses VEGFR2 promoter activity to inhibit angiogenesis and that E2- 2–mediated EC inactivation can be alleviated through interaction with Id. Methods. Plasmids and adenovirusesc. DNAs for human and mouse E2- 2 as well as mouse LMO2 were cloned by reverse- transcription polymerase chain reaction (RT- PCR). Each c. DNA was sequenced before use. Mouse stem cell leukemia hematopoietic transcription factor (SCL) was a kind gift from Dr M. Ema (University of Tsukuba, Japan). DNAs were inserted into Flag- pc. DNA3 or Myc- pc. DNA3. DEF3 vector. 2. 9 DEF3- Flag- Id. DEF3- Myc- Id. 1, and DEF3- Id. MCKpfos- luc and p. GL2b- VEGFR2- luc (. Sigvardsson (Lund University, Sweden) and C. Hughes (University of California, Irvine), respectively. VEGFR2- luc mutant constructs were also generated by PCR. After verification of each sequence, reporter constructs were used for each experiment. Adenoviruses expressing Myc- E2- 2 were generated using the p. Ad. Track- CMV vector. After recombination of p. Ad. Track- CMV- Myc- E2- 2 with p. Ad. Easy- 1,3. 2 the resulting plasmid was transfected into 2. T cells, and adenoviruses were amplified. Adenoviruses expressing Flag- Id. Cell culture. COS7 cells and mouse embryonic endothelial cells (MEECs)1. Dulbecco modified Eagle medium (DMEM; Invitrogen) containing 1. FCS; Invitrogen), minimum essential medium nonessential amino acids (Invitrogen), and 1. U/m. L penicillin/streptomycin (Wako). Calf pulmonary aortic endothelial cells (CPAEs)3. DMEM with 1. 0% FCS, 2. M N- 2- hydroxyethylpiperazine- N. Primary human umbilical vein endothelial cells (HUVECs) were cultured in endothelial basal medium (Lonza Walkersville) supplemented with 2% FCS. MEECs and HUVECs were grown on 0. Adenoviral infections. Adenoviruses were incubated in DMEM containing polybrene (Sigma- Aldrich; 8. Two hours after infection, cells were washed and allowed to recover 2. If necessary, cells were starved by removal from the FCS overnight and then stimulated with 5. L recombinant human VEGF (Wako). Immunoprecipitation and Western blotting. To detect interactions among the proteins, plasmids were transfected into COS7 cells (5 . Forty hours after transfection, the cells were lysed in 5. Cell lysates were precleared with protein G- Sepharose beads (GE Healthcare) for 3. Protein complexes were immunoprecipitated by incubation with protein G- Sepharose beads for 3. Immunoprecipitated proteins and aliquots of total cell lysates were boiled for 5 minutes in sample buffer, separated by sodium dodecyl sulfate- polyacrylamide gel electrophoresis, and transferred to Hybond- C Extra membranes (GE Healthcare). The membranes were probed with anti- Myc 9. E1. 0 antibody (Santa Cruz Biotechnology). Primary antibodies were detected using horseradish peroxidase- conjugated goat anti–mouse antibody (GE Healthcare) and chemiluminescent substrate (Thermo Electron). Protein expression in total cell lysates was evaluated by Western blotting using anti- Flag M5 or anti- Myc 9. E1. 0 antibody. To detect the endogenous interaction between Id. E2- 2, either an anti–E2- 2 monoclonal antibody (anti- TCF4 M0. Abnova) or an anti- Id. Santa Cruz Biotechnology) was used. RNA isolation and RT- PCRTotal RNA was isolated using the RNeasy kit (QIAGEN). Reverse transcription was carried out using a First- Strand c. DNA Synthesis Kit (Takara). PCR was performed using Taq polymerase (Invitrogen) as directed by the manufacturer. Primer sets used are shown in supplemental Tables 1 and 2 (available on the Blood Web site; see the Supplemental Materials link at the top of the online article). Transcriptional reporter assay. MEECs were seeded at 5 . After 4. 0 hours of transfection, lysates were prepared and luciferase activity was measured using a luciferase assay system (Promega). Results were corrected by measuring . Each experiment was carried out in triplicate and repeated at least twice. Values represent the mean plus or minus SD (n = 3). Immunofluorescence. Immunofluorescence assay was performed as previously described. Briefly, MEECs grown on the cover glass were stimulated with 2. L BMP6 to induce Id. After treatment, the glasses were washed once with phosphate- buffered saline (PBS), fixed for 1. PFA; Wako), washed 3 times with PBS, subsequently permeabilized with 0. Triton X- 1. 00 in PBS for 5 minutes, and washed again 3 times with PBS. Glasses were blocked with 5% normal swine serum (Dako Denmark) in PBS at 3. The glasses were then washed 3 times with PBS, incubated with 5% normal swine serum (in PBS) including both fluorescein isothiocyanate- conjugated goat anti–mouse Ig. G antibody (diluted 1: 2. Invitrogen) and Texas red- conjugated goat anti–rabbit Ig. G antibody (diluted 1: 2. Invitrogen) at room temperature for 1 hour, and washed 3 times with PBS. To visualize the fluorescence, an immunofluorescence microscope (Axiovert 2. M; Carl Zeiss) was used. Migration assay. Cell migration assays were performed using a Boyden chamber. Costar nucleopore filters (8- . The chambers were washed 3 times with PBS. Adenovirus- infected HUVECs starved for 1. FCS were added to the top of each migration chamber at a density of 1. Angiogenesis - Wikipedia. Angiogenesis is the physiological process through which new blood vessels form from pre- existing vessels. The first vessels in the developing embryo form through vasculogenesis, after which angiogenesis is responsible for most, if not all, blood vessel growth during development and in disease. However, it is also a fundamental step in the transition of tumors from a benign state to a malignant one, leading to the use of angiogenesis inhibitors in the treatment of cancer. The essential role of angiogenesis in tumor growth was first proposed in 1. Judah Folkman, who described tumors as . It occurs in several well- characterized stages. First, biological signals known as angiogenic growth factors activate receptors on endothelial cells present in pre- existing blood vessels. Second, the activated endothelial cells begin to release enzymes called proteases that degrade the basement membrane to allow endothelial cells to escape from the original (parent) vessel walls. The endothelial cells then proliferate into the surrounding matrix and form solid sprouts connecting neighboring vessels. As sprouts extend toward the source of the angiogenic stimulus, endothelial cells migrate in tandem, using adhesion molecules called integrins. These sprouts then form loops to become a full- fledged vessel lumen as cells migrate to the site of angiogenesis. Sprouting occurs at a rate of several millimeters per day, and enables new vessels to grow across gaps in the vasculature. It is markedly different from splitting angiogenesis because it forms entirely new vessels as opposed to splitting existing vessels. Intussusceptive angiogenesis. In this type of vessel formation, the capillary wall extends into the lumen to split a single vessel in two. There are four phases of intussusceptive angiogenesis. First, the two opposing capillary walls establish a zone of contact. Second, the endothelialcell junctions are reorganized and the vessel bilayer is perforated to allow growth factors and cells to penetrate into the lumen. Third, a core is formed between the 2 new vessels at the zone of contact that is filled with pericytes and myofibroblasts. These cells begin laying collagen fibers into the core to provide an extracellular matrix for growth of the vessel lumen. Finally, the core is fleshed out with no alterations to the basic structure. Intussusception is important because it is a reorganization of existing cells. It allows a vast increase in the number of capillaries without a corresponding increase in the number of endothelial cells. This is especially important in embryonic development as there are not enough resources to create a rich microvasculature with new cells every time a new vessel develops. There is a significant amount of controversy with regard to shear stress acting on capillaries to cause angiogenesis, although current knowledge suggests that increased muscle contractions may increase angiogenesis. Nitric oxide results in vasodilation of blood vessels. Chemical stimulation. In general, FGFs stimulate a variety of cellular functions by binding to cell surface FGF- receptors in the presence of heparin proteoglycans. The FGF- receptor family is composed of seven members, and all the receptor proteins are single- chain receptor tyrosine kinases that become activated through autophosphorylation induced by a mechanism of FGF- mediated receptor dimerization. Receptor activation gives rise to a signal transduction cascade that leads to gene activation and diverse biological responses, including cell differentiation, proliferation, and matrix dissolution, thus initiating a process of mitogenic activity critical for the growth of endothelial cells, fibroblasts, and smooth muscle cells. FGF- 1, unique among all 2. FGF family, can bind to all seven FGF- receptor subtypes, making it the broadest- acting member of the FGF family, and a potent mitogen for the diverse cell types needed to mount an angiogenic response in damaged (hypoxic) tissues, where upregulation of FGF- receptors occurs. FGF- 2 is a more potent angiogenic factor than VEGF or PDGF (platelet- derived growth factor); however, it is less potent than FGF- 1. As well as stimulating blood vessel growth, a. FGF (FGF- 1) and b. FGF (FGF- 2) are important players in wound healing. They stimulate the proliferation of fibroblasts and endothelial cells that give rise to angiogenesis and developing granulation tissue; both increase blood supply and fill up a wound space/cavity early in the wound- healing process. Vascular endothelial growth factor (VEGF) has been demonstrated to be a major contributor to angiogenesis, increasing the number of capillaries in a given network. Initial in vitro studies demonstrated bovine capillary endothelial cells will proliferate and show signs of tube structures upon stimulation by VEGF and b. FGF, although the results were more pronounced with VEGF. Binding to VEGF receptor- 2 (VEGFR- 2) starts a tyrosine kinase signaling cascade that stimulates the production of factors that variously stimulate vessel permeability (e. NOS, producing NO), proliferation/survival (b. FGF), migration (ICAMs/VCAMs/MMPs) and finally differentiation into mature blood vessels. Mechanically, VEGF is upregulated with muscle contractions as a result of increased blood flow to affected areas. The increased flow also causes a large increase in the m. RNA production of VEGF receptors 1 and 2. The increase in receptor production means muscle contractions could cause upregulation of the signaling cascade relating to angiogenesis. As part of the angiogenic signaling cascade, NO is widely considered to be a major contributor to the angiogenic response because inhibition of NO significantly reduces the effects of angiogenic growth factors. However, inhibition of NO during exercise does not inhibit angiogenesis, indicating there are other factors involved in the angiogenic response. These receptors are tyrosine kinases. Thus, they can initiate cell signaling when ligand binding causes a dimerization that initiates phosphorylation on key tyrosines. Another major contributor to angiogenesis is matrix metalloproteinase (MMP). MMPs help degrade the proteins that keep the vessel walls solid. This proteolysis allows the endothelial cells to escape into the interstitial matrix as seen in sprouting angiogenesis. Inhibition of MMPs prevents the formation of new capillaries. The presence of blood vessels where there should be none may affect the mechanical properties of a tissue, increasing the likelihood of failure. The absence of blood vessels in a repairing or otherwise metabolically active tissue may inhibit repair or other essential functions. Several diseases, such as ischemic chronic wounds, are the result of failure or insufficient blood vessel formation and may be treated by a local expansion of blood vessels, thus bringing new nutrients to the site, facilitating repair. Other diseases, such as age- related macular degeneration, may be created by a local expansion of blood vessels, interfering with normal physiological processes. The modern clinical application of the principle of angiogenesis can be divided into two main areas: anti- angiogenic therapies, which angiogenic research began with, and pro- angiogenic therapies. Whereas anti- angiogenic therapies are being employed to fight cancer and malignancies. One of the first applications of pro- angiogenic methods in humans was a German trial using fibroblast growth factor 1 (FGF- 1) for the treatment of coronary artery disease. Difficulties include effective integration of the therapeutic genes into the genome of target cells, reducing the risk of an undesired immune response, potential toxicity, immunogenicity, inflammatory responses, and oncogenesis related to the viral vectors used in implanting genes and the sheer complexity of the genetic basis of angiogenesis. The most commonly occurring disorders in humans, such as heart disease, high blood pressure, diabetes and Alzheimer's disease, are most likely caused by the combined effects of variations in many genes, and, thus, injecting a single gene may not be significantly beneficial in such diseases. In contrast, pro- angiogenic protein therapy uses well- defined, precisely structured proteins, with previously defined optimal doses of the individual protein for disease states, and with well- known biological effects. Oral, intravenous, intra- arterial, or intramuscular routes of protein administration are not always as effective, as the therapeutic protein may be metabolized or cleared before it can enter the target tissue. Cell- based pro- angiogenic therapies are still early stages of research, with many open questions regarding best cell types and dosages to use. Tumor angiogenesis. A malignant tumor consists of a population of rapidly dividing and growing cancer cells that progressively accrues mutations. However, tumors need a dedicated blood supply to provide the oxygen and other essential nutrients they require in order to grow beyond a certain size (generally 1. Growth factors such as b. FGF and VEGF can induce capillary growth into the tumor, which some researchers suspect supply required nutrients, allowing for tumor expansion. Unlike normal blood vessels, tumor blood vessels are dilated with an irregular shape. In normal cells (but not in cancerous ones), PKG apparently limits beta- catenin, which solicits angiogenesis. In either case, angiogenesis is a necessary and required step for transition from a small harmless cluster of cells, often said to be about the size of the metal ball at the end of a ball- point pen, to a large tumor. Angiogenesis is also required for the spread of a tumor, or metastasis. Single cancer cells can break away from an established solid tumor, enter the blood vessel, and be carried to a distant site, where they can implant and begin the growth of a secondary tumor.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
May 2017
Categories |
 RSS Feed
RSS Feed
